The general term for bulges or sacs that form in the large intestine, or colon, is diverticular disease.
While any part of the colon can be affected, it's usually the area of the large intestine closest to the rectum where these sacs develop most often. If left untreated, diverticular disease has the potential to lead to serious complications.
What Is Diverticular Disease?
Diverticular disease can be broken down into two more specific conditions: diverticulosis and diverticulitis. Diverticulitis refers to the development of small sacs or pockets ("diverticula") that form within the bowel lining. Diverticula are larger irregular formations. They develop in weak spots within walls of the intestine due to pressure from gas or waste. They can also form as a result of excessive bowel straining, like what happens when experiencing constipation, especially if it's chronic or recurring in nature.
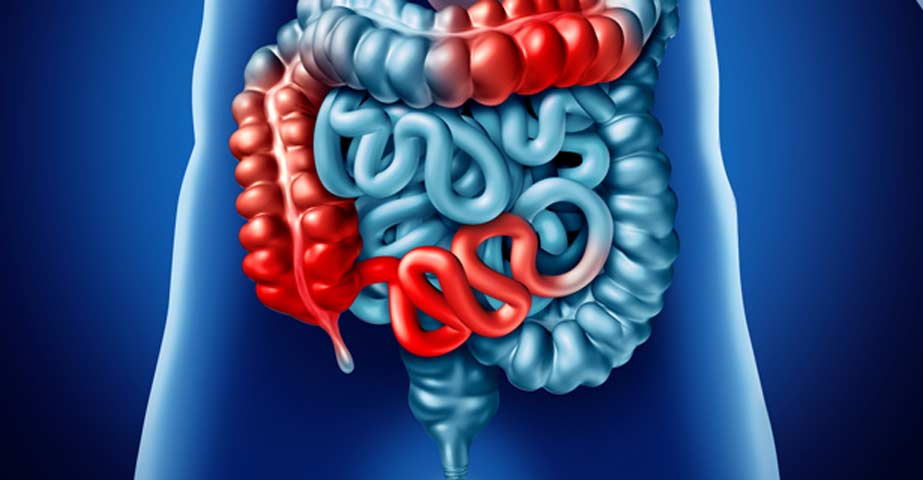
What Are Possible Symptoms?
Diverticulosis does not usually produce symptoms that are all that disruptive or severe. Symptoms, when they do occur, may include abdominal pain or cramping or tenderness within or around the affected area. Diverticulitis tends to produce more noticeable and severe symptoms, some of which may include cramps that are painful or persistent and lower abdominal tenderness. Some patients also experience fever and chills. Diverticulitis has the potential to lead to serious complications, some of which may include:
- Abscesses
- Intestinal blockages
- Peritonitis
How Is a Diagnosis Made?
Since symptoms related to diverticulosis are usually mild, this particular form of diverticular disease often remains undiagnosed until image or rectal-related testing is done for another reason. With diverticulitis, there is typically a need to rule out other conditions that can produce similar symptoms, such as irritable bowel syndrome (IBS) and ulcers.
Diagnosis of either form of diverticular disease may involve ultrasound scans, CT scans, and similar types of image tests, a discussion of bowel habits, a colonoscopy or sigmoidoscopy, and a barium enema. Blood tests may also be done to look for signs of infection. If rectal bleeding is the main symptom, an angiography may be done to determine the source of the bleeding.
What Are Treatment Options?
Diverticulosis not producing symptoms may not require any treatment other than regular observation during routine exams. However, patients are often encouraged to consider a high-fiber diet. Diverticulitis may be treated with IV antibiotics if there is an infection present. While an active infection exists, a patient may be advised to reduce fiber intake and drink more water. Fiber can then be reintroduced after the infection has cleared up.
Abscesses may be drained with a needle. If the infection is severe, surgery may be necessary to remove part of the colon or remove multiple abscesses. Surgery is also typically needed if peritonitis has developed and spread to the abdominal cavity.
The most effective way to reduce the possibility of developing diverticular disease is to practice good bowel hygiene. This generally involves avoiding excessive bowel straining, making healthy diet choices to reduce issues with constipation, getting regular exercise, and drinking sufficient water daily. With fiber intake, the standard recommendation is 20 to 35 grams of fiber per day.

